XCOPRI TITRATION
Flexible, once-daily XCOPRI dosing as monotherapy and adjunctive therapy1
XCOPRI IS TITRATED AT 2-WEEK INTERVALS. TITRATION PACKS ARE AVAILABLE TO SIMPLIFY TITRATION.
START
Begin with the initial 12.5 mg/25 mg titration pack
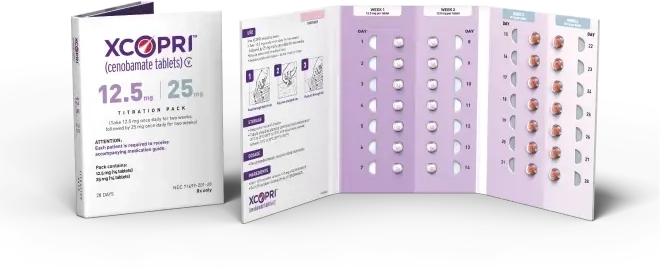
Weeks 1-4
CONTINUE
Titrate using the 50 mg/100 mg titration pack
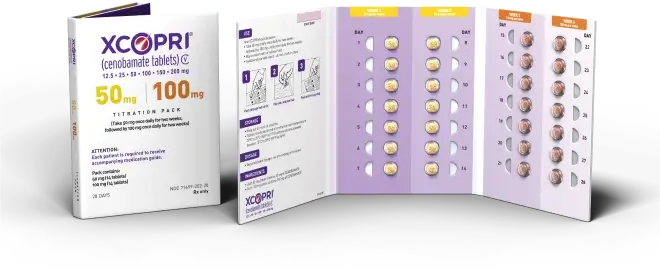
Weeks 5-8
IF ADDITIONAL SEIZURE
REDUCTION IS NEEDED
For patients who require more than 100 mg, dosage may be increased by 50 mg/day every two weeks to a maximum of 400 mg/day*
Effective dosage range 100 mg ‑ 400 mg
XCOPRI may be taken any time, whole or crushed, with or without food.
Patients with mild or moderate hepatic impairment: 200 mg/day is the maximum dosage. XCOPRI is not recommended for use in patients with severe hepatic impairment.
See Full Prescribing Information for additional Dosage and Administration instructions.
XCOPRI ONCE-DAILY DOSING
Flexibility for a personal approach—from titration to maintenance dosing
XCOPRI Titration Blister Packs
Designed to simplify the titration schedule of XCOPRI. At-a-glance instructions have been included to assist you and your patients as XCOPRI dosages are increased over time.1

12.5 mg/25 mg (28-day supply)

50 mg/100 mg (28-day supply)
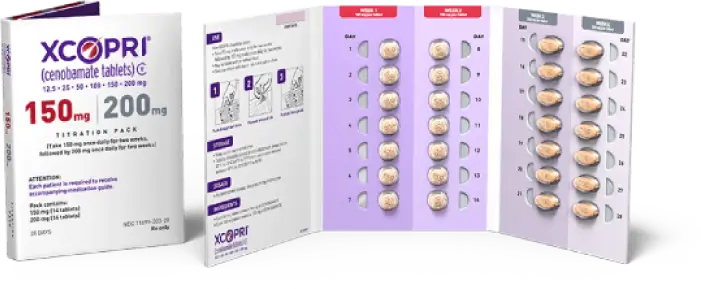
150 mg/200 mg (28-day supply)
XCOPRI Bottles
Designed to give you the flexibility to find the dosage that is right for your individual patients.1
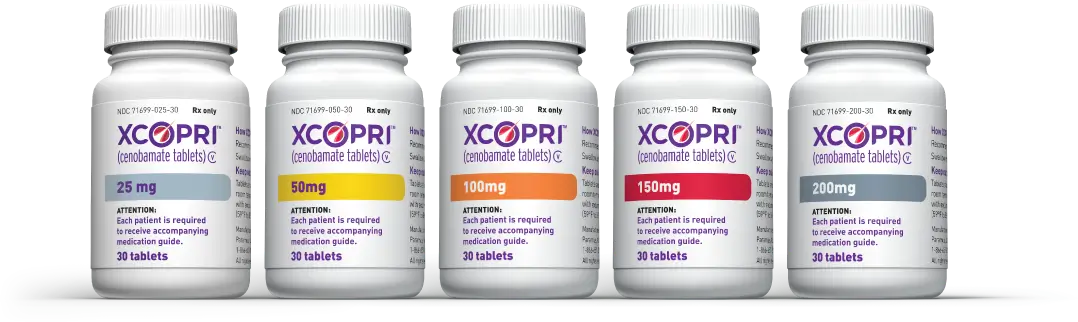
Maintenance bottles available:
• 25 mg (30-count bottle)
• 50 mg (30-count bottle)
• 100 mg (30-count bottle)
• 150 mg (30-count bottle)
• 200 mg (30-count bottle)
XCOPRI Maintenance Blister Packs
Designed to give you the flexibility to find the dosage that is right for your individual patients.1
Maintenance blister
packs available:
• 250 mg [28-day supply]
• 350 mg [28-day supply]
ANTI-SEIZURE MEDICATION (ASM) DOSING CONSIDERATIONS
Using XCOPRI with other ASMs
XCOPRI makes the concentration of some drugs go up. Consider decreasing the dosage of clobazam, phenytoin, and phenobarbital early in XCOPRI titration.1,2
(anti-seizure medication)
If a patient experiences common adverse events, consider decreasing the dosage of other ASMs.1,2
XCOPRI can be used as monotherapy and adjunctive therapy
Watch this video to learn more about ASM dosing considerations when adding XCOPRI to a patient’s treatment regimen
In this interactive video, watch as Lawrence Seiden, MD, and Barry Gidal, PharmD, discuss anti-seizure medication (ASM) dosing considerations to be aware of when adding XCOPRI to a patient’s treatment regimen. Discover essential information regarding the optimization of XCOPRI’s efficacy, plus potential ways to minimize side effects—and be sure to bookmark for reference.
Find more information for prescribing XCOPRI with concomitant medications